Difference between revisions of "Neuropathology tumours"
Jensflorian (talk | contribs) (sort + update ganglioglioma (needs split out in future)) |
Jensflorian (talk | contribs) (little sorting) |
||
| Line 5: | Line 5: | ||
==Brain tumours - overview== | ==Brain tumours - overview== | ||
===Adult=== | ===Alphabetical=== | ||
For overview see [[:Category:Neuropathology_tumours|here]] | |||
===By age group=== | |||
====Adult==== | |||
Four most common types of brain tumours:<ref>[http://neurosurgery.mgh.harvard.edu/abta/primer.htm http://neurosurgery.mgh.harvard.edu/abta/primer.htm]</ref> | Four most common types of brain tumours:<ref>[http://neurosurgery.mgh.harvard.edu/abta/primer.htm http://neurosurgery.mgh.harvard.edu/abta/primer.htm]</ref> | ||
# Metastatic brain tumours (barely edges out primary tumours) | # Metastatic brain tumours (barely edges out primary tumours) | ||
| Line 16: | Line 20: | ||
# [[Meningioma]]. | # [[Meningioma]]. | ||
===Children=== | ====Children==== | ||
# Pilocytic astrocytoma. | # [[Pilocytic astrocytoma]]. | ||
# [[Medulloblastoma]]. | # [[Medulloblastoma]]. | ||
# [[Ependymoma]]. | # [[Ependymoma]]. | ||
| Line 23: | Line 27: | ||
===Location (most common)=== | ===Location (most common)=== | ||
Certain tumours like to hang-out at certain places:<ref>URL: [http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/files/4ce563fb7e8e48fc9ed8b42e296a7747.gif http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/files/4ce563fb7e8e48fc9ed8b42e296a7747.gif] and [http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/sid117213.html http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/sid117213.html]. Accessed on: 2 November 2010.</ref> | Certain tumours like to hang-out at certain places:<ref>URL: [http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/files/4ce563fb7e8e48fc9ed8b42e296a7747.gif http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/files/4ce563fb7e8e48fc9ed8b42e296a7747.gif] and [http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/sid117213.html http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/sid117213.html]. Accessed on: 2 November 2010.</ref> | ||
====Cerebrum==== | |||
**Cortical based - [[oligodendroglioma]]. | **Cortical based - [[oligodendroglioma]]. | ||
**Grey-white junction - metastases. | **Grey-white junction - metastases. | ||
| Line 29: | Line 33: | ||
**Periventricular - CNS lymphoma. | **Periventricular - CNS lymphoma. | ||
**Cystic - [[ganglioglioma]], [[pilocytic astrocytoma]], [[pleomorphic xanthoastrocytoma]]. | **Cystic - [[ganglioglioma]], [[pilocytic astrocytoma]], [[pleomorphic xanthoastrocytoma]]. | ||
====Cerebellum==== | |||
**Midline/central - [[medulloblastoma]]. | **Midline/central - [[medulloblastoma]]. | ||
**Cystic lesion - pilocytic astrocytoma (younger individual), [[hemangioblastoma]] (older individual). | **Cystic lesion - pilocytic astrocytoma (younger individual), [[hemangioblastoma]] (older individual). | ||
**Solid lesion (older individual) - [[metastasis]]. | **Solid lesion (older individual) - [[metastasis]]. | ||
====Spinal cord==== | |||
**[[Ependymoma]], glioblastoma. | **[[Ependymoma]], glioblastoma. | ||
**Filum terminale - [[myxopapillary ependymoma]], [[paraganglioma]]. | **Filum terminale - [[myxopapillary ependymoma]], [[paraganglioma]]. | ||
====Filum terminale==== | ====Filum terminale==== | ||
*Filum terminale = bottom end of the spinal cord - has a limited differential. | *Filum terminale = bottom end of the spinal cord - has a limited differential. | ||
DDx:<ref>JLK. 31 May 2010.</ref> | DDx:<ref>JLK. 31 May 2010.</ref> | ||
*[[Meningioma]]. | *[[Meningioma]]. | ||
| Line 49: | Line 51: | ||
====Cerebellopontine angle==== | ====Cerebellopontine angle==== | ||
*Abbreviated ''CP angle''. | *Abbreviated ''CP angle''. | ||
DDx:<ref>R. Kiehl. 8 November 2010.</ref> | DDx:<ref>R. Kiehl. 8 November 2010.</ref> | ||
*[[Schwannoma]]. | *[[Schwannoma]]. | ||
| Line 248: | Line 249: | ||
*IDH1 and IDH2 mutations - better survival.<ref name=pmid20975057>{{cite journal |author=Houillier C, Wang X, Kaloshi G, ''et al.'' |title=IDH1 or IDH2 mutations predict longer survival and response to temozolomide in low-grade gliomas |journal=Neurology |volume=75 |issue=17 |pages=1560–6 |year=2010 |month=October |pmid=20975057 |doi=10.1212/WNL.0b013e3181f96282 |url=}}</ref> | *IDH1 and IDH2 mutations - better survival.<ref name=pmid20975057>{{cite journal |author=Houillier C, Wang X, Kaloshi G, ''et al.'' |title=IDH1 or IDH2 mutations predict longer survival and response to temozolomide in low-grade gliomas |journal=Neurology |volume=75 |issue=17 |pages=1560–6 |year=2010 |month=October |pmid=20975057 |doi=10.1212/WNL.0b013e3181f96282 |url=}}</ref> | ||
== | ==Astrocytic tumours== | ||
{{Main| | {{Main|Astrocytoma}} | ||
* Diffuse [[Astrocytoma]] | |||
* [[Anaplastic astrocytoma]] | |||
* [[Glioblastoma]] | |||
* [[Gliomatosis cerebri]] | |||
* [[Pilocytic astrocytoma]] (PA) | |||
* [[Pilomyxoid astrocytoma]] (PMA) | |||
* [[Pleomorphic xanthoastrocytoma]] (PXA) | |||
* [[Subependymal giant cell astrocytoma]] (SEGA) | |||
== | ==Oligodendroglial tumours== | ||
* | * [[Oligodendroglioma]] | ||
* Anaplastic oligodendroglioma | |||
* [[Oligoastrocytoma]] | |||
* Anaplastic oligoastrocytoma | |||
== | ==Ependymal tumours== | ||
* | * [[Subependymoma]] | ||
* [[Myxopapillary Ependymoma]] | |||
* [[Ependymoma]] | |||
* Anaplastic ependymoma | |||
== | ==Choroid plexus tumours== | ||
* [[Choroid plexus papilloma]] | |||
* Atypical choroid plexus papilloma | |||
* [[Choroid plexus carcinoma]] | |||
== | ==Other neuroepithelial tumours== | ||
* Astroblastoma | |||
* Chordoid glioma of the third ventricle | |||
* [[Angiocentric glioma]] | |||
== | ===Astroblastoma=== | ||
*No WHO grade yet. | |||
*Very rare superficial tumor of young age. | |||
*Large, cystic. Pushing margin towards CNS. | |||
*Vasocentric growth, plump cells with absence of fibrillary pattern. | |||
*GFAP+ve, Synaptohysin-ve, focally EMA/panCK+ve. MIB-1: 1-18 %. | |||
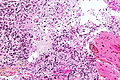
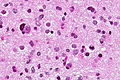
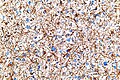
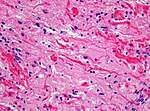
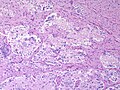
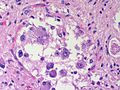
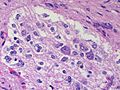
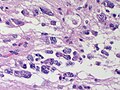
<gallery> | |||
File:Astroblastoma_HE_Specimen.jpg | HE. (WC/jensflorian) | |||
File:Astroblastoma_HE_papillae.jpg | HE. (WC/jensflorian) | |||
File:Astroblastoma.jpg | Astroblastoma (AFIP) | |||
</gallery> | |||
==Chordoid glioma of the | ===Chordoid glioma of the third ventricle=== | ||
* WHO grade II. | * WHO grade II. | ||
* Slowly growing, non-invasive. | * Slowly growing, non-invasive. | ||
| Line 296: | Line 304: | ||
* GFAP+ve, MIB-1 1-3%. | * GFAP+ve, MIB-1 1-3%. | ||
==Gangliocytoma== | ==Neuronal and mixed neuronal/glial tumours== | ||
* Desmoplastic infantile astrocytoma / ganglioglioma (DIA/DIG) | |||
* [[Dysembryoplastic neuroepithelial tumour]] | |||
* [[Central Neurocytoma]] / Extraventricular [[neurocytoma]] | |||
* Cerebellar liponeurocytoma | |||
* Papillary glioneuronal tumour | |||
* Rosette-forming glioneuronal tumour of the fourth ventricle | |||
* Gangliocytoma / Ganglioglioma | |||
* Dysplastic ganglioglioma of the cerebellum (Lhermitte-Duclos) | |||
* [[Paraganglioma]] | |||
===Gangliocytoma=== | |||
* Grade I WHO neuronal tumour. | * Grade I WHO neuronal tumour. | ||
** ICD-O code: 9492/0 | ** ICD-O code: 9492/0 | ||
| Line 302: | Line 321: | ||
* Non-neoplastic, reticulin-rich glial stroma. | * Non-neoplastic, reticulin-rich glial stroma. | ||
==Ganglioglioma== | ===Ganglioglioma=== | ||
:'''Not''' to be confused with ''[[ganglioneuroma]]''. | :'''Not''' to be confused with ''[[ganglioneuroma]]''. | ||
===General=== | ====General==== | ||
*Grade I WHO mixed neuronal-glial tumour. | *Grade I WHO mixed neuronal-glial tumour. | ||
*ICD-O code: 9505/1 (Anaplastic ganglioglioma: 9505/3) | *ICD-O code: 9505/1 (Anaplastic ganglioglioma: 9505/3) | ||
| Line 311: | Line 330: | ||
*Recognized as a cause of [[epilepsy]].<ref name=pmid12125968>{{Cite journal | last1 = Im | first1 = SH. | last2 = Chung | first2 = CK. | last3 = Cho | first3 = BK. | last4 = Lee | first4 = SK. | title = Supratentorial ganglioglioma and epilepsy: postoperative seizure outcome. | journal = J Neurooncol | volume = 57 | issue = 1 | pages = 59-66 | month = Mar | year = 2002 | doi = | PMID = 12125968 }}</ref> | *Recognized as a cause of [[epilepsy]].<ref name=pmid12125968>{{Cite journal | last1 = Im | first1 = SH. | last2 = Chung | first2 = CK. | last3 = Cho | first3 = BK. | last4 = Lee | first4 = SK. | title = Supratentorial ganglioglioma and epilepsy: postoperative seizure outcome. | journal = J Neurooncol | volume = 57 | issue = 1 | pages = 59-66 | month = Mar | year = 2002 | doi = | PMID = 12125968 }}</ref> | ||
===Microscopic=== | ====Microscopic==== | ||
Features: | Features: | ||
*Dysplastic neurons. | *Dysplastic neurons. | ||
| Line 325: | Line 344: | ||
*Necrosis | *Necrosis | ||
===IHC=== | ====IHC==== | ||
*Neurons: | *Neurons: | ||
**[[MAP2]] +ve | **[[MAP2]] +ve | ||
| Line 333: | Line 352: | ||
**CD34+/-ve | **CD34+/-ve | ||
===DDx:=== | ====DDx:==== | ||
*[[DNT]]. | *[[DNT]]. | ||
*[[Oligodendroglioma]]. | *[[Oligodendroglioma]]. | ||
*Trapped cortical neurons in diffuse astrocytoma. | *Trapped cortical neurons in diffuse astrocytoma. | ||
===Images=== | ====Images==== | ||
<gallery> | <gallery> | ||
File:Ganglioglioma lymphocytic cuffing PAS.jpg | Lymphocytic cuffing in ganglioglioma (WC/jensflorian) | File:Ganglioglioma lymphocytic cuffing PAS.jpg | Lymphocytic cuffing in ganglioglioma (WC/jensflorian) | ||
| Line 347: | Line 366: | ||
*[http://path.upmc.edu/cases/case282.html Ganglioglioma - case 2 (upmc.edu)]. | *[http://path.upmc.edu/cases/case282.html Ganglioglioma - case 2 (upmc.edu)]. | ||
===Lhermitte-Duclos disease=== | |||
*Abbreviated ''LDD''. | |||
*[[AKA]] ''dysplastic cerebellar gangliocytoma''.<ref name=pmid20060133>{{Cite journal | last1 = Yağci-Küpeli | first1 = B. | last2 = Oguz | first2 = KK. | last3 = Bilen | first3 = MA. | last4 = Yalçin | first4 = B. | last5 = Akalan | first5 = N. | last6 = Büyükpamukçu | first6 = M. | title = An unusual cause of posterior fossa mass: Lhermitte-Duclos disease. | journal = J Neurol Sci | volume = 290 | issue = 1-2 | pages = 138-41 | month = Mar | year = 2010 | doi = 10.1016/j.jns.2009.12.010 | PMID = 20060133 }}</ref> | |||
*[[AKA]] ''dysplastic gangliocytoma of the cerebellum''. | |||
{{Main|Lhermitte-Duclos disease}} | |||
== | ==Pineal tumours== | ||
{{Main|Pineal gland}} | |||
{{Main| | |||
* [[Pineocytoma]] | |||
* [[Pineal parenchymal tumour of intermediate differentiation]] | |||
* | * [[Pineoblastoma]] | ||
* | * [[Papillary tumour of the pineal region]] | ||
== | ==Embryonal tumours== | ||
* [[Atypical teratoid/rhabdoid tumour]] (AT/RT) or (AT-RT) | |||
* [[Medulloblastoma]] | |||
* [[Primitive neuroectodermal tumour]] (PNET) | |||
* | * [[Embryonal tumour with abundant neuropil and true rosettes]] (ETANTR) | ||
==Peripheral nerve sheath tumours== | ==Peripheral nerve sheath tumours== | ||
{{Main|Peripheral nerve sheath tumours}} | {{Main|Peripheral nerve sheath tumours}} | ||
A classification:<ref name=pmid17893219>{{cite journal |author=Wippold FJ, Lubner M, Perrin RJ, Lämmle M, Perry A |title=Neuropathology for the neuroradiologist: Antoni A and Antoni B tissue patterns |journal=AJNR Am J Neuroradiol |volume=28 |issue=9 |pages=1633–8 |year=2007 |month=October |pmid=17893219 |doi=10.3174/ajnr.A0682 |url=http://www.ajnr.org/cgi/reprint/28/9/1633}}</ref> | A classification:<ref name=pmid17893219>{{cite journal |author=Wippold FJ, Lubner M, Perrin RJ, Lämmle M, Perry A |title=Neuropathology for the neuroradiologist: Antoni A and Antoni B tissue patterns |journal=AJNR Am J Neuroradiol |volume=28 |issue=9 |pages=1633–8 |year=2007 |month=October |pmid=17893219 |doi=10.3174/ajnr.A0682 |url=http://www.ajnr.org/cgi/reprint/28/9/1633}}</ref> | ||
'''Benign:''' | |||
*[[Schwannoma]]. | |||
*[[Neurofibroma]]. | |||
*[[Perineurioma]]. | |||
*Ganglioneuroma. | |||
**[[Traumatic neuroma]]. | **[[Traumatic neuroma]]. | ||
'''Malignant:''' | |||
*[[Malignant peripheral nerve sheath tumour]] (MPNST). | |||
==Ganglioneuroma== | ===Ganglioneuroma=== | ||
:'''Not''' to be confused with ''[[ganglioglioma]]''. | :'''Not''' to be confused with ''[[ganglioglioma]]''. | ||
*[[AKA]] ganglioma.<ref>URL: [http://medical-dictionary.thefreedictionary.com/ganglioma http://medical-dictionary.thefreedictionary.com/ganglioma]. Accessed on: 8 November 2010.</ref> | *[[AKA]] ganglioma.<ref>URL: [http://medical-dictionary.thefreedictionary.com/ganglioma http://medical-dictionary.thefreedictionary.com/ganglioma]. Accessed on: 8 November 2010.</ref> | ||
{{Main|Ganglioneuroma}} | {{Main|Ganglioneuroma}} | ||
==Meningioma== | |||
{{Main|Meningioma}} | |||
==Chordoma== | ==Chordoma== | ||
| Line 456: | Line 456: | ||
*Bcl-6 +ve. | *Bcl-6 +ve. | ||
*Bcl-1 -ve. | *Bcl-1 -ve. | ||
==Ganglioneuroblastoma== | ==Ganglioneuroblastoma== | ||
Revision as of 13:41, 14 October 2015
The article covers tumours in neuropathology. Tumours are a large part of neuropathology. Cytopathology of CNS tumours is dealt with in the article CNS cytopathology.
There are separate articles for peripheral nerve sheath tumours and pituitary/peri-pituitary lesions.
Brain tumours - overview
Alphabetical
For overview see here
By age group
Adult
Four most common types of brain tumours:[1]
- Metastatic brain tumours (barely edges out primary tumours)
- Lung (most common).
- Breast.
- Melanoma.
- Renal cell carcinoma (RCC).
- Glioblastoma (previously known as glioblastoma multiforme).
- Anaplastic astrocytoma.
- Meningioma.
Children
Location (most common)
Certain tumours like to hang-out at certain places:[2]
Cerebrum
- Cortical based - oligodendroglioma.
- Grey-white junction - metastases.
- White matter - astrocytoma, glioblastoma.
- Periventricular - CNS lymphoma.
- Cystic - ganglioglioma, pilocytic astrocytoma, pleomorphic xanthoastrocytoma.
Cerebellum
- Midline/central - medulloblastoma.
- Cystic lesion - pilocytic astrocytoma (younger individual), hemangioblastoma (older individual).
- Solid lesion (older individual) - metastasis.
Spinal cord
- Ependymoma, glioblastoma.
- Filum terminale - myxopapillary ependymoma, paraganglioma.
Filum terminale
- Filum terminale = bottom end of the spinal cord - has a limited differential.
DDx:[3]
Cerebellopontine angle
- Abbreviated CP angle.
DDx:[4]
- Schwannoma.
- Meningioma.
- Dermoid cyst/epidermoid cyst.
- Ependymoma.
- Choroid plexus papilloma.
Cystic tumours
DDx:[5]
- Pilocytic astrocytoma.
- Pleomorphic xanthoastrocytoma.
- Ganglioglioma.
- Hemangioblastoma.
- Craniopharyngioma.[6]
Primary versus secondary
- AKA (primary) brain tumour versus metastatic cancer.
Primary
Glial tumours:
- Cytoplasmic processes - key feature.
- Best seen at highest magnification - usu. ~1 micrometer.
- Processes may branch.
- Ill-defined border/blend with the surrounding brain.
- Large (lymphoid) cells, ergo usu. not a difficult diagnosis.
- ~2x size of resting lymphocyte, nucleoli.
- Lesion predominantly perivascular.
Secondary
Carcinomas:
- Well-demarcated border between brain and lesion - key feature.
- No cytoplasmic processes.
- Usu. have nuclear atypia of malignancy.
- Nuclei often ~3-4x the size of a RBC.
- +/-Glandular arrangement.
- +/-Nucleoli.
Common neuropathology tumours in a table
| Type | Key feature(s) | Imaging | History | Notes | IHC | Images |
| Normal tissue | cells regularly spaced, no nuc. atypia | small lesion? / deep lesion? | variable | missed lesion? | nil | |
| Reactive astrocytes | astrocytes with well-demarcated eosinophilic cytoplasm, regular spacing, no nuc. atypia | small lesion? / deep lesion? | variable | missed lesion / close to a lesion; non-specific pathologic process - need more tissue | nil | |
| Schwannoma | cellular areas (Antoni A), paucicelluar areas (Antoni B), palisading of nuclei (Verocay bodies) | extra-axial + intradural | old or young | need frozen section to Dx, DDx: meningioma | S100 | |
| Meningioma | whorls, psammomatous calcs, nuclear inclusions | extra-axial + intradural | old or young | may be diagnosed on smear, DDx: schwannoma, choroid plexus | EMA, PR, Ki-67 | |
| Infiltrative astrocytoma (WHO grade II or grade III) | glial processes (esp. on smear), nuclear atypia (typical size var. ~3x, irreg. nuc. membrane, hyperchromasia), no Rosenthal fibres in the core of the lesion †, no microvascular proliferation, no necrosis | often enhancing (suggests high grade), usu. supratentorial, usu. white matter | usu. old, occ. young | common | IDH-1+/-, GFAP+ | |
| Glioblastoma (WHO grade IV) | glial processes (esp. on smear), nuclear atypia (typical size var. ~3x, irreg. nuc. membrane, hyperchromasia), no Rosenthal fibres in the core of the lesion †, microvascular proliferation or necrosis | often enhancing (suggests high grade), usu. supratentorial, usu. white matter | usu. old, occ. young | very common, esp. glioblastoma | IDH-1+/-, GFAP+ | |
| Metastasis | sharp interface with brain, often glandular, +/-nucleoli, no glial processes | often cerebellular, well-circumscribed | usu. old | often suspected to have metastatic disease | TTF-1, CK7, CK20, BRST-2 |
† Rosenthal fibres at the periphery of a lesion are a non-specific finding seen in chronic processes.
Brain metastasis
Infiltrative astrocytomas
Overview
- Low-grade (diffuse) astrocytomas (WHO Grade II).
- Anaplastic astrocytomas (WHO Grade III).
- Glioblastoma(WHO Grade IV).
- Gliosarcoma (WHO Grade IV).
- Gliomatosis cerebri (Grade III/IV).
Notes:
- Non-infiltrative astrocytomas:
- Pilocytic astrocytoma (WHO Grade I).
- Pilomyxoid astrocytoma (WHO Grade II).
- Pleomorphic xanthoastrocytoma (WHO grade II).
- Subependymal giant cell astrocytoma (WHO grade I).
- Pilocytic astrocytoma (WHO Grade I).
Microscopic
- Glial processes - key feature.
- Thin stringy cytoplasmic processes - best seen at high power in less cellular areas.
- No Rosenthal fibres within the tumour itself.
Images:
- Endothelial proliferation in a GBM (ouhsc.edu).
- Endothelial proliferation (ouhse.edu).
- Gemistocytic astrocytoma - several images (upmc.edu).
Notes:
- Glial vs. non-glial tumours:
- Glial: "blends into brain"/gradual transition to non-tumour brain.
- Non-glial: no glial processes.
- Rosenthal fibres within the tumour... make it into a pilocytic astrocytoma.
- Rosenthal fibres may be seen around a (very) slow growing tumour and represent a reactive process.
- Inflammatory cells and macrophages should prompt consideration of an alternate diagnosis (e.g. cerebral infarct, multiple sclerosis) - esp. if this is a primary lesion.[9]
Grading
Nuclear pleomorphism present:
- At least grade II (diffuse astrocytoma).
Mitotic figures present:
- At least grade III (anaplastic astrocytoma).
Microvascular proliferation or necrosis with pseudopalisading tumour cells:
- Grade IV (glioblastoma AKA glioblastoma multiforme).
Notes:
- Pseudopalisading tumour cells = high tumour cell density adjacent to regions of necrosis; palisade = a fence of poles forming a defensive barrier or fortification.
Images
Glioblastoma:
Anaplastic astrocytoma:
Table of common gliomas - grading
Histomorphologic comparison of common gliomas:
| Entity | Rosenthal fibres / EGBs |
Nuclear atypia | Mitoses | Necrosis or MVP | Infiltrative | Image |
| Pilocytic astrocytoma | yes | usu. no | usu. no | usu. no | no | |
| Low-grade astrocytoma | no | yes | no | no | yes | |
| Anaplastic astrocytoma | no | yes | yes | no | yes | |
| Glioblastoma | no | yes | yes | yes | yes |
Notes:
- MVP = microvascular proliferation.
- EGBs = eosinophilic granular bodies.
IHC
- GFAP - should stain cytoplasm of tumour cells and the perikaryon (nuclear membrane).
- Ki-67 - usu. high >20% of cells.
- p53 - often +ve.
- IDH1 (isocitrate dehydrogenase 1).
- +ve in tumours that arose from low-grade gliomas.[10]
- Image: IDH1 +ve in glioblastoma (WP).
- +ve in tumours that arose from low-grade gliomas.[10]
Notes:
- IDH1 and IDH2 mutations - better survival.[11]
Astrocytic tumours
- Diffuse Astrocytoma
- Anaplastic astrocytoma
- Glioblastoma
- Gliomatosis cerebri
- Pilocytic astrocytoma (PA)
- Pilomyxoid astrocytoma (PMA)
- Pleomorphic xanthoastrocytoma (PXA)
- Subependymal giant cell astrocytoma (SEGA)
Oligodendroglial tumours
- Oligodendroglioma
- Anaplastic oligodendroglioma
- Oligoastrocytoma
- Anaplastic oligoastrocytoma
Ependymal tumours
- Subependymoma
- Myxopapillary Ependymoma
- Ependymoma
- Anaplastic ependymoma
Choroid plexus tumours
- Choroid plexus papilloma
- Atypical choroid plexus papilloma
- Choroid plexus carcinoma
Other neuroepithelial tumours
- Astroblastoma
- Chordoid glioma of the third ventricle
- Angiocentric glioma
Astroblastoma
- No WHO grade yet.
- Very rare superficial tumor of young age.
- Large, cystic. Pushing margin towards CNS.
- Vasocentric growth, plump cells with absence of fibrillary pattern.
- GFAP+ve, Synaptohysin-ve, focally EMA/panCK+ve. MIB-1: 1-18 %.
Chordoid glioma of the third ventricle
- WHO grade II.
- Slowly growing, non-invasive.
- Clusters of epithelioid cells in mucinous stroma.
- Lymphocytic infiltrates, adjacent Rosenthal fibers.
- Few mitoses.
- GFAP+ve, MIB-1 1-3%.
Neuronal and mixed neuronal/glial tumours
- Desmoplastic infantile astrocytoma / ganglioglioma (DIA/DIG)
- Dysembryoplastic neuroepithelial tumour
- Central Neurocytoma / Extraventricular neurocytoma
- Cerebellar liponeurocytoma
- Papillary glioneuronal tumour
- Rosette-forming glioneuronal tumour of the fourth ventricle
- Gangliocytoma / Ganglioglioma
- Dysplastic ganglioglioma of the cerebellum (Lhermitte-Duclos)
- Paraganglioma
Gangliocytoma
- Grade I WHO neuronal tumour.
- ICD-O code: 9492/0
- Groups of irregular large neurons.
- Non-neoplastic, reticulin-rich glial stroma.
Ganglioglioma
- Not to be confused with ganglioneuroma.
General
- Grade I WHO mixed neuronal-glial tumour.
- ICD-O code: 9505/1 (Anaplastic ganglioglioma: 9505/3)
- Rare.
- Usu. temporal lobe.
- Recognized as a cause of epilepsy.[12]
Microscopic
Features:
- Dysplastic neurons.
- Out of regular architecture / abnormal location.
- Cytomegaly
- Clustering
- Binucleated (very occassionally).
- Atypical glia.
- Calcification.
- Lymphocytic cuffing.
Anaplastic ganglioglioma:
- Brisk mitotic activity
- Necrosis
IHC
- Neurons:
- MAP2 +ve
- Synaptophysin +ve
- Neurofilament +ve
- Glia:
- CD34+/-ve
DDx:
- DNT.
- Oligodendroglioma.
- Trapped cortical neurons in diffuse astrocytoma.
Images
Lhermitte-Duclos disease
- Abbreviated LDD.
- AKA dysplastic cerebellar gangliocytoma.[13]
- AKA dysplastic gangliocytoma of the cerebellum.
Pineal tumours
- Pineocytoma
- Pineal parenchymal tumour of intermediate differentiation
- Pineoblastoma
- Papillary tumour of the pineal region
Embryonal tumours
- Atypical teratoid/rhabdoid tumour (AT/RT) or (AT-RT)
- Medulloblastoma
- Primitive neuroectodermal tumour (PNET)
- Embryonal tumour with abundant neuropil and true rosettes (ETANTR)
Peripheral nerve sheath tumours
A classification:[14] Benign:
- Schwannoma.
- Neurofibroma.
- Perineurioma.
- Ganglioneuroma.
Malignant:
Ganglioneuroma
- Not to be confused with ganglioglioma.
Meningioma
Chordoma
Hemangioblastoma
CNS lymphoma
Classification:
- Primary CNS lymphoma.
- Non-primary CNS lymphoma - see lymphoma article.
General - primary CNS
- Classically periventicular distribution.
- Usually large B cell; can be considered a type of diffuse large B cell lymphoma (DLBCL).
- Prognosis of CNS (DLBCL) lymphomas worse than nodal (non-CNS) DLBCL.[16]
Microscopic
Features:
- Large cell lymphoma.
- Size = 2x diameter normal lymphocyte.
- Nucleolus - common.
- Perivascular clustering.
Images
www:
IHC
Can be subclassified in GCB (germinal centre B-cell-like) and non-GCB by CD10, Bcl-6, MUM1/IRF-4, and Bcl-2.[16]
Common pattern:
- CD20 +ve - key stain.
- CD3 -ve.
- Ki-67 ~40%.
- Bcl-6 +ve.
- Bcl-1 -ve.
Ganglioneuroblastoma
General
- Uncommon.
- Part of the neuroblastic tumours group which includes:[17]
- Ganglioneuroma (benign).
- Ganglioneuroblastoma (intermediate).
- Neuroblastoma (aggressive).
Microscopic
Features:
- Ganglion-like cells with a prominent nucleolus.
- Small undifferentiated cells with scant cytoplasm.
Images:
IHC
- NSE +ve -- small cells.
Lesions of the sella turcica
Lesions of the sella turcica, the pituitary gland environs, is a topic for it self. The differential diagnosis for lesions in this area includes:
- Pituitary adenoma.
- Craniopharyngioma.
- Rathke cleft cyst.
- Germ cell tumour.
- Meningioma.
- Pilomyxoid astrocytoma - in children.
See also
References
- ↑ http://neurosurgery.mgh.harvard.edu/abta/primer.htm
- ↑ URL: http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/files/4ce563fb7e8e48fc9ed8b42e296a7747.gif and http://www.msdlatinamerica.com/ebooks/DiagnosticNeuropathologySmears/sid117213.html. Accessed on: 2 November 2010.
- ↑ JLK. 31 May 2010.
- ↑ R. Kiehl. 8 November 2010.
- ↑ URL: http://path.upmc.edu/cases/case320/dx.html. Accessed on: 14 January 2012.
- ↑ URL: http://www.pathologyoutlines.com/Cnstumor.html#cystsgeneral. Accessed on: 14 January 2012.
- ↑ Rong Y, Durden DL, Van Meir EG, Brat DJ (June 2006). "'Pseudopalisading' necrosis in glioblastoma: a familiar morphologic feature that links vascular pathology, hypoxia, and angiogenesis". J. Neuropathol. Exp. Neurol. 65 (6): 529–39. PMID 16783163.
- ↑ http://dictionary.reference.com/browse/palisading
- ↑ URL: http://path.upmc.edu/cases/case79/dx.html. Accessed on: 2 January 2012.
- ↑ Yan H, Parsons DW, Jin G, et al. (February 2009). "IDH1 and IDH2 mutations in gliomas". N. Engl. J. Med. 360 (8): 765–73. doi:10.1056/NEJMoa0808710. PMC 2820383. PMID 19228619. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2820383/.
- ↑ Houillier C, Wang X, Kaloshi G, et al. (October 2010). "IDH1 or IDH2 mutations predict longer survival and response to temozolomide in low-grade gliomas". Neurology 75 (17): 1560–6. doi:10.1212/WNL.0b013e3181f96282. PMID 20975057.
- ↑ Im, SH.; Chung, CK.; Cho, BK.; Lee, SK. (Mar 2002). "Supratentorial ganglioglioma and epilepsy: postoperative seizure outcome.". J Neurooncol 57 (1): 59-66. PMID 12125968.
- ↑ Yağci-Küpeli, B.; Oguz, KK.; Bilen, MA.; Yalçin, B.; Akalan, N.; Büyükpamukçu, M. (Mar 2010). "An unusual cause of posterior fossa mass: Lhermitte-Duclos disease.". J Neurol Sci 290 (1-2): 138-41. doi:10.1016/j.jns.2009.12.010. PMID 20060133.
- ↑ Wippold FJ, Lubner M, Perrin RJ, Lämmle M, Perry A (October 2007). "Neuropathology for the neuroradiologist: Antoni A and Antoni B tissue patterns". AJNR Am J Neuroradiol 28 (9): 1633–8. doi:10.3174/ajnr.A0682. PMID 17893219. http://www.ajnr.org/cgi/reprint/28/9/1633.
- ↑ URL: http://medical-dictionary.thefreedictionary.com/ganglioma. Accessed on: 8 November 2010.
- ↑ 16.0 16.1 Raoux D, Duband S, Forest F, et al. (June 2010). "Primary central nervous system lymphoma: Immunohistochemical profile and prognostic significance". Neuropathology 30 (3): 232–40. doi:10.1111/j.1440-1789.2009.01074.x. PMID 19925562.
- ↑ Shimada H, Ambros IM, Dehner LP, Hata J, Joshi VV, Roald B (July 1999). "Terminology and morphologic criteria of neuroblastic tumors: recommendations by the International Neuroblastoma Pathology Committee". Cancer 86 (2): 349–63. PMID 10421272.